Understanding Lipedema: A Comprehensive Guide From Treatment to Recovery
For countless women, the frustrating reality of bulging fatty tissue in the hips and legs is all too familiar – a struggle that can take an immense toll on confidence and well-being.
This could be lipedema, a chronic condition causing a buildup of fatty tissue, typically in the legs, calves, hips, and buttocks areas. Often misunderstood or misdiagnosed, lipedema’s symmetric buildup of non-removable fat in these areas can be frustrating.
If you’ve found yourself feeling helpless in the face of this condition, you’re not alone. But there’s hope.
This guide is your roadmap to understanding lipedema. We’ll explore treatment options, management strategies, and how to feel your best again despite having this condition.
What is Lipedema?
If you’re a woman who has struggled with bulging fatty deposits in your legs and hips that just won’t go away no matter how much you diet or exercise, you may be dealing with lipedema.
As mentioned above, this chronic condition causes an abnormal buildup of fat cells, primarily in the lower body. Sometimes, it also affects the arms.
Lipedema is more common than you might think. Research estimates it affects up to 11% of women worldwide.
Yet, it frequently goes undiagnosed or misdiagnosed due to a lack of awareness. Many women are unknowingly living with this condition, left feeling frustrated and helpless.
Causes
While the exact causes are still being investigated, we know lipedema has ties to hormones and genetics. The condition runs in families in up to 60% of cases, suggesting a genetic predisposition.
Lipedema also seems to be triggered or exacerbated by hormonal changes like puberty, pregnancy, and menopause.
Another possible correlation is obesity, as most people with this condition have a BMI above 35. However, more studies are needed to confirm this.
Symptoms
The key symptom of lipedema is the buildup of fatty tissue in the lower body that creates a disproportionate, column-like appearance between the upper body and lower body.
Some other common signs include:
- Difference in size between feet and legs
- Easy bruising and pain in the fatty areas
- Tenderness and a heavy feeling in the legs
- Skin that has a dimpled or “floppy” texture
- Feeling like there are bumps inside the fat
- Presence of varicose veins in the affected areas
- Swelling that worsens in the afternoon, evening, hot weather, or after doing activities
- Fatigue
As lipedema progresses through stages, excessive fat accumulates from the hips down to the ankles, upper arms become affected, and mobility issues can arise due to joint pain.
Stages
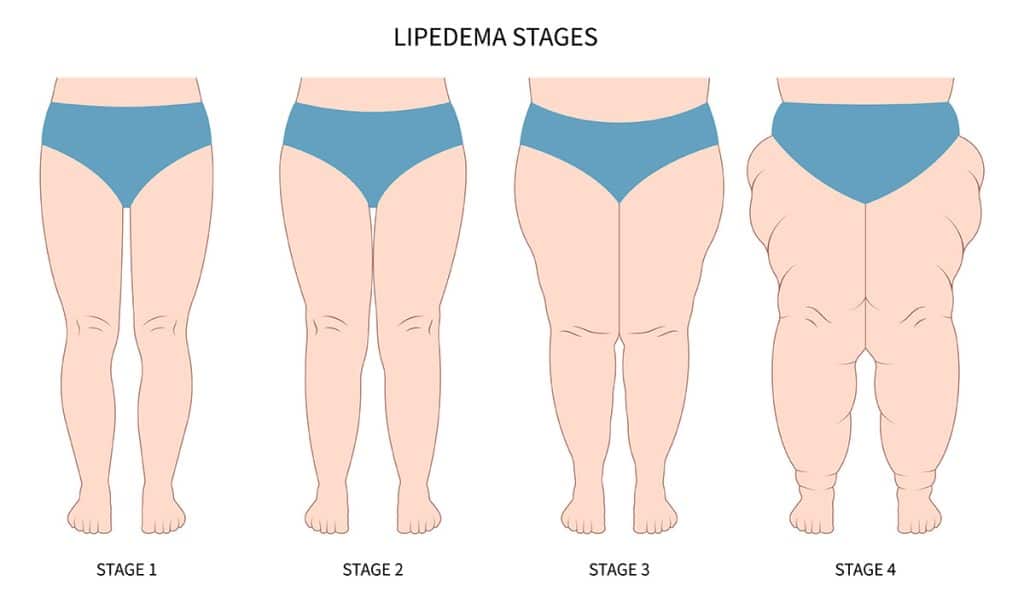
There are five stages of lipedema that indicate severity:
- Stage 0: No visible swelling, but has a general feeling of heaviness and pain
- Stage 1: No visible swelling, but feeling that there’s something underneath the skin
- Stage 2: Skin looks uneven or bumpy
- Stage 3: Large folds of skin and fat, especially on the legs, making moving around hard.
- Stage 4: Already coupled with lymphedema; swelling throughout the lower body and arms
What is the Difference Among Lipedema, Obesity, and Lymphedema?
It might be confusing, but lipedema is different from obesity and lymphedema.
While obesity causes weight gain, lipedema is localized fat buildup on the lower body.
Meanwhile, lymphedema stems from fluid accumulation due to lymphatic dysfunction, thus affecting only one side of the body, including the hands and feet. Lipedema is a proliferation of fat cells and manifests mainly on the lower extremities.
How is Lipedema Diagnosed?
Diagnosing lipedema can be tricky since its symptoms overlap with other conditions like obesity or lymphedema. Many women go years without a proper diagnosis, leaving them frustrated and without targeted treatment. That’s why seeing a trained medical professional who can accurately identify lipedema is essential.
There is not one test that can definitively diagnose lipedema. Instead, doctors rely on various diagnostic tools like a physical examination, medical history review, and ruling out other potential causes through imaging tests.
Physical Exam
During the physical exam, your doctor looks for critical signs of lipedema, such as painful, dense, fatty areas with a distinctive texture and slimmer feet and hands. They may perform techniques like the “Stemmer sign,” where they pinch the skin on your toe — thick skin can indicate lymphedema rather than lipedema.
Imaging Scans
Imaging scans such as MRIs, CT scans, ultrasounds, or DEXA bone density tests allow your doctor to visualize the fatty deposits and check for abnormalities.
How is Lipedema Treated?
While there is no cure for lipedema yet, several conservative treatment options can help manage symptoms and improve your quality of life.
Non-Invasive Approaches
Healthy Diet and Exercise
A balanced, anti-inflammatory diet can provide overall health benefits for lipedema. It should contain fruits, vegetables, lean proteins, and healthy fats.
However, it’s essential to have realistic expectations because dieting alone won’t reduce lipedema fat.
Low-impact exercises like swimming, walking, and stationary cycling are also recommended. They promote mobility, increase lymphatic drainage, and reduce inflammation without putting too much strain on your joints.
Be sure to tailor your exercise routine based on your capabilities.
Compression Therapy
Compression garments like stockings, leggings, or arm sleeves can significantly relieve swelling and discomfort associated with lipedema. The gentle, sustained pressure helps improve circulation and prevent further fluid buildup in affected areas.
Your doctor can prescribe properly fitted medical compression wear.
Manual Lymphatic Drainage (MLD)
MLD is a specialized massage technique that uses gentle pumping motions to remove stagnant lymph fluid and reduce swelling. It redirects fluid away from blocked areas toward healthy lymph vessels where it can properly drain.
MLD mitigates pain and may prevent tissue hardening over time when done regularly.
Complex Decongestive Therapy
You may combine MLD with compression therapy using complex decongestive therapy to ease pain. This involves lymphatic drainage massage, compression, exercise, and meticulous skin and nail care.
Skincare
Use a skin moisturizer to prevent your skin from drying out. Also, taking care of your skin can reduce your risk of wounds and infections.
Surgical Approaches
For some women, conservative treatments like compression therapy and lifestyle changes may not provide enough relief from lipedema’s symptoms.
In these cases, surgical interventions like liposuction can be considered.
Liposuction
Liposuction surgically removes the abnormal, painful fat deposits that characterize lipedema.
Advanced techniques like tumescent liposuction are often recommended, as they are less likely to damage the lymphatic system than traditional methods. Multiple sessions may be needed depending on the amount of fat involved.
While liposuction can significantly reduce lipedema fat and the associated pain and mobility issues, it does not cure the underlying condition. The fat can potentially re-accumulate over time.
Ensuring Liposuction Results
Many plastic surgeons look at lipedema solely as a medical condition — it has to be treated even without regard for the aesthetic consequences. That’s why consulting with a qualified plastic surgeon experienced in liposuction, lipedema treatments, and skin removal surgeries, like Dr. Siamak Agha, is crucial.
Dr. Agha understands that removing fat is essential, as is the technique used. After all, lipedema involves the removal of a significant amount of fat, resulting in skin laxity. Thus, the more fat removed via liposuction, the worse the skin laxity and contour irregularities might become.
That is why it’s vital to go to a plastic surgeon and body contouring expert who can perform optimal liposuction and plan for the consequential skin removal many patients need. This prevents unwanted results, such as contour irregularities, depression, and asymmetry.
Insurance Coverage
Great news: insurance coverage for lipedema has become more attainable in recent years.
Whereas lipedema surgery was previously often dismissed as purely cosmetic, many insurance companies now recognize it as a medically necessary treatment when specific criteria are met. They typically require documented evidence of symptoms like:
- Painful swelling and disproportionate fat accumulation in the limbs
- Easy bruising and dimpled “orange peel” skin texture
- Lack of improvement with weight loss efforts alone
Your primary care physician needs to provide detailed medical records, including photographs clearly showing the hallmarks of lipedema, during a physical exam. Demonstrating how the condition significantly impairs your mobility and daily functioning is also important.
Additionally, most insurers want to see that you’ve first tried at least three months of conservative treatments like compression therapy and massage without adequate relief before approving surgery.
Bariatric Surgery
For women with both lipedema and obesity (BMI over 35), bariatric surgeries like gastric bypass may be an option.
Some research indicates these procedures can help reduce overall leg volume and lipedema symptoms and promote weight loss.
Be sure to have an open discussion with your doctor about whether you are a good candidate and understand the full scope of recovery involved.
Living with Lipedema
Coping with lipedema goes far beyond just managing the physical symptoms. The painful swelling, mobility limitations, and body image struggles are more than just inconveniences — they can profoundly impact your self-esteem and mental well-being.
That’s why self-care is so crucial. Connecting with others who understand what you’re going through in a support group setting can provide invaluable solidarity and tips for thriving with lipedema. Working with a counselor can also help develop healthy coping strategies.
While gentle exercise like swimming aids lymphatic drainage, modifying higher-impact activities and investing in comfortable, compression garments increase your mobility and confidence. Little adjustments, like wearing breathable fabrics and avoiding restrictive clothing, go a long way.
Don’t forget about lymphatic massages as part of your lymphedema management routine. The light, rhythmic motions facilitate fluid drainage to minimize swelling.
Be patient and compassionate with yourself along the way.
Conclusion
You don’t have to face the challenges of lipedema alone.
At The Aesthetic Centers, our caring, experienced team has helped many women reclaim their lives from this condition. With our deep expertise in the latest lipedema treatments and management approaches, we’re committed to providing you with a personalized plan that delivers thorough, sustainable relief.
We understand this isn’t a one-size-fits-all journey, so schedule a consultation with Dr. Agha so we can examine your case and outline a clear path forward, giving you the tools to feel like your best self again.
Lipedema FAQs
Can I be obese and have lipedema?
The short answer is yes — these two conditions may exist simultaneously.
But while obesity and lipedema can sometimes look similar, especially in the lower body areas, it’s crucial to understand their differences.
Lipedema is characterized by a buildup of abnormal fat cells that primarily affects the legs, hips, and arms in a symmetrical pattern – leaving areas like the feet unaffected. Obesity, on the other hand, causes overall weight gain throughout the entire body.
If you think you may have lipedema, consult with a healthcare professional for proper evaluation and diagnosis. They can assess the distinct characteristics distinguishing lipedema from obesity, such as painful fat deposits, easy bruising, and lack of response to weight loss efforts in the affected areas.
Will insurance cover my liposuction for lipedema treatment?
With the proper documentation from your physician, getting lipedema surgery covered is becoming more attainable.
You simply need to provide evidence, medical records with photographs, and demonstrate how lipedema impairs your daily functioning.
How long will recovery take after surgery?
Expect 4-6 weeks of recovery with activity restrictions to allow proper healing.
Learn more about Lipedema:







